Treatment Options
Depending on the severity and extent of your symptoms and your goals, you and your healthcare practitioner can discuss the various treatment options.
Stress Incontinence
- Pelvic floor muscle rehabilitation – pelvic muscle exercises, also known as Kegel exercise, can help reduce or eliminate urine leakage. Just like other exercises, technique and dedication to regularly performing the exercises will yield the best results.
- Surgical treatments – a number of minimally invasive surgical procedures may be performed, and surgery has the highest cure rate, even in elderly women.
Bladder neck slings
Burch laparoscopic bladder neck suspension - Bulking agents - Injectable urethral bulking agents are used for treatment of stress urinary incontinence. Improvement is achieved by increasing the tissue bulk around the urethra and thereby increasing resistance to the outflow of urine.
- Vaginal Pessaries – A pessary is a plastic device that can be fitted to help support prolapsed pelvic organs and may help with incontinence. When fitted properly, it should be comfortable and allow you to urinate and have bowel movements without any difficulty. Many women will use a pessary if they want to delay surgery, or avoid having surgery. For more information on pessaries....
- InTone - a customized device from InControl Medical that uses muscle stimulation, active resistance and biofeedback to increase muscle strength in the pelvic floor.
- FemSoft urethral plug - A small one-time-use urethral insert available by prescription. The insert is used only when needed to control urine leakage. Our healthcare practitioners can help determine if FemSoft is right for you. We will fit you with the correct size and teach you how to use it. At your appointment, your clinician will provide you instructions and samples to help you get started. Femsoft works by temporarily obstructing the urethra. It provides immediate relief from stress related incontinence and can be used continuously or occasionally to meet your needs. Depending on your frequency of use, you can expect to feel confident using FemSoft on your own within a couple days to two weeks.
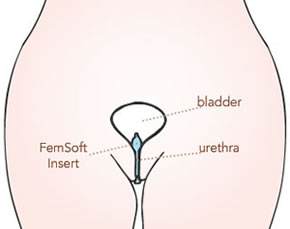 |
FemSoft is a small, single-use product, available by prescription and currently the only urethral insert for sale in the U.S. Once you insert FemSoft into your urethra, it gives you immediate control over unwanted urine loss, odor, and wetness–without surgery or medication. A long-term FemSoft study showed that 93% of women were completely dry when using FemSoft, and 95% said they would recommend it to a friend. Find answers to frequently asked questions. |
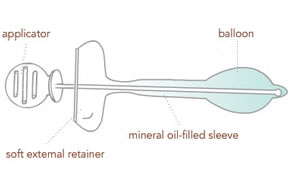 |
FemSoft consists of a narrow silicone tube that's encased in a soft, pliable, mineral oil-filled sleeve. To protect delicate tissue, the FemSoft Insert is smooth and seamless, with no hard surfaces. The insert conforms to your body, creating such a comfortable fit that users report hardly knowing it's there. |
Urge Incontinence
- Dietary modifications – certain foods and drinks can cause women to go to the bathroom more frequently. Working with your healthcare provider, you may be able to identify bladder irritants (like caffeine, alcohol, artificial sweeteners). Constipation can also make urgency and frequency worse, so increased dietary fiber can help.
- Bladder training – By retraining your bladder to hold more urine, urges can be better controlled. This is done by learning to go to the bathroom at specific intervals, and also learning strategies to control urges.
- Medications – For more severe cases of urge incontinence, medication may be required. Medication provides the best results when it is combined with bladder training and dietary modifications.
- Neurostimulation – Nerves located in the lower back affect your bladder. We can perform a simple test to see if your symptoms are affected by these nerves. Evaluations can be performed in the hospital or practitioner’s office. Following evaluation, treatment involves placing a small nerve stimulation device; this can be performed in a minor daystay procedure. For more information, click here.
- InTone - a customized device from InControl Medical that uses muscle stimulation, active resistance and biofeedback to increase muscle strength in the pelvic floor.
Additional Resources:
- Voices for Pelvic Floor Disorders
- Stress and Urge Incontinence Treatments (UptoDate for Patients)
- Cleveland Clinic’s Pelvic Organ Prolapse and Incontinence Treatment Guide
- National Association for Continence
- Hypoallergenic Reusable Pads
- InControl Medical, makers of the InTone device for urinary incontinence





